Key Takeaways
- Burn injuries create complex adaptive system disruptions spanning molecular to societal scales with emergent properties unpredictable from single components.
- Computational modeling tools (network analysis, agent-based models, systems dynamics) can capture multiscale interactions in burn wound healing.
- A paradigm shift from reductionist to complexity science approaches is essential for advancing burn care research and clinical outcomes.
TL;DR
Burn care has evolved from focusing solely on survival to addressing quality of life across physical, mental, and social dimensions. Severe burn injuries disrupt multiple interconnected systems - from cellular metabolism to patient psychology - creating unpredictable emergent behaviors like burn shock that cannot be understood by studying individual components alone. Traditional reductionist approaches fail to capture these dynamic interactions, leaving clinicians unable to accurately predict outcomes for complex cases involving comorbidities and multifactorial influences. The authors propose applying complexity science and systems biology to model burn care across multiscale levels (molecular to societal). Using computational tools like network analysis, agent-based modeling, and causal loop diagrams, researchers can visualize hidden patterns in wound healing dynamics. This holistic approach enables better prediction of tipping points in patient conditions, supports personalized treatment strategies, and bridges gaps between preclinical research and clinical practice, ultimately improving decision-making in burn centers.
Why Does It Matter?
This paper introduces a paradigm shift from traditional reductionist medical models to complexity science frameworks, offering researchers novel methodological tools for studying complex adaptive systems in healthcare. By demonstrating how multiscale modeling and systems biology approaches can bridge preclinical research and clinical practice, it provides a roadmap for understanding emergent phenomena like burn shock and scar formation. The emphasis on computational tools - including network analysis and agent-based modeling - enables researchers to quantify uncertainty and predict nonlinear system behaviors, potentially revolutionizing personalized burn treatment strategies and disaster management protocols.
Multi-Scaling
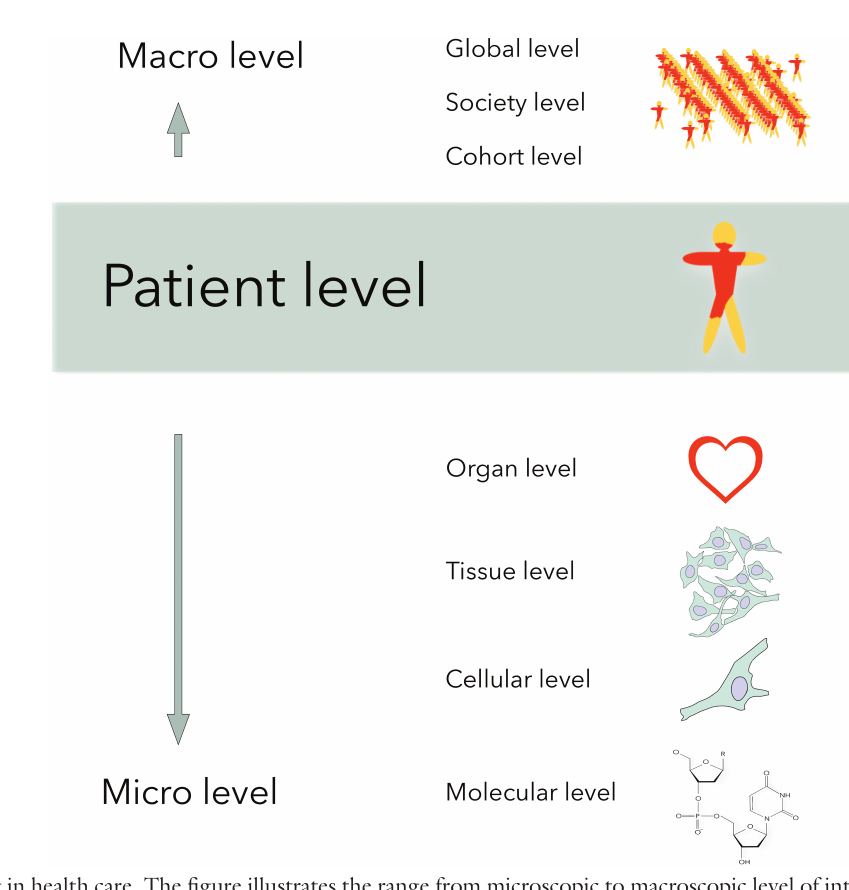
The concept of multi-scaling represents a fundamental characteristic of complex adaptive systems in burn care, describing how biological processes operate across hierarchical levels from molecular micro-scales through tissues to patient macro-scales. As shown in Figure 1, the body functions as a nested system where microscopic interactions cascade upward to influence macroscopic outcomes, while feedback loops modulate lower levels. Table 1 notes that organs comprise cellular subsystems interacting across micro-, meso-, and macro-scales. In burn healing, temporal multi-scaling spans microseconds for signaling to years for scar maturation, while spatial multi-scaling ranges from nanometer proteins to decimeter organs. This necessitates computational models coupling interactions across vastly different scales, as reductionist approaches fail to capture emergent properties from cross-scale interactions in burn injuries.
CAS Framework
The paper positions Complex Adaptive Systems (CAS) as a transformative lens for burn care, emphasizing that biological and organizational systems operate through emergent properties arising from countless agent interactions rather than linear chains. Key insights reveal that severe burns disrupt nested CAS hierarchies - from molecular to societal levels - triggering nonlinear responses like systemic inflammation that cannot be predicted by analyzing isolated components. The framework illuminates why reductionist approaches fall short, advocating instead for computational modeling and agent-based simulations that capture self-organization and path dependency. Particularly compelling is the application of CAS to multidisciplinary burn teams themselves, suggesting these structures must function as adaptive learning systems with continuous feedback loops. Embracing unpredictability and multi-scaling dynamics - acknowledging that micro-level cellular behaviors cascade to macro-level outcomes - is essential for personalized medicine and improving long-term quality of life.
Nonlinear Logic
Nonlinearity represents a fundamental characteristic of complex adaptive systems that challenges traditional linear causality in burn care. Unlike proportional input-output relationships, nonlinear logic reveals how subtle initial variations - such as minor cytokine fluctuations or microvascular permeability changes - can cascade through interconnected biological networks, triggering disproportionate systemic consequences like burn shock or abrupt organ failure. This manifests through tipping points where stable homeostasis suddenly shifts to crisis states, creating inherent unpredictability despite comprehensive knowledge of individual components. The paper emphasizes that burn wound healing exhibits emergent behaviors where collective outcomes transcend isolated pathway summations, necessitating clinicians abandon reductionist single-factor interventions for dynamic, multiscale strategies that accommodate the body's complex adaptive nature and its capacity for disproportionate responses to stressors.
Agent Models
Agent-based models represent a powerful computational paradigm within complexity science that specifically addresses the spatial limitations inherent in traditional network and system dynamics approaches to modeling burn wound healing. By treating cells as autonomous agents - such as fibroblasts and granulocytes that exhibit chemotaxis and secrete collagen - these models operate within discrete simulation domains to capture location-based interactions and emergent spatial patterns that deterministic equations cannot adequately represent. Through multiscale integration with system dynamics frameworks, they enable comprehensive exploration of healing trajectories from initial immune responses through vasculature development to final scar formation. This approach proves invaluable for understanding how spatial heterogeneity - including wound geometry and vasculature proximity - influences clinical outcomes, offering predictive insights into scar formation patterns that could guide targeted therapeutic interventions in complex adaptive burn care systems.
Tipping Points
The concept of tipping points represents a profound insight from complexity science that fundamentally challenges traditional linear medical models. As delineated in Table 1, tipping points occur in complex adaptive systems when sudden, unpredictable transitions emerge after periods of apparent stability, where the system abruptly shifts from one state to another. In burn care contexts, this manifests clinically when patients suddenly become hemodynamically unstable after appearing stable, illustrating how incremental physiological changes can trigger disproportionate systemic collapse. This phenomenon underscores the nonlinear dynamics inherent in burn injury pathophysiology, where the interaction of inflammatory mediators, cellular responses, and organ systems creates emergent behaviors that cannot be predicted by examining individual components alone. Recognizing tipping points requires clinicians to view patients as integrated complex systems rather than assemblies of isolated organs, necessitating adaptive monitoring strategies that account for potential abrupt transitions. Understanding these critical thresholds illuminates why early intervention is crucial before the system crosses irreversible boundaries, offering a framework for developing more resilient clinical protocols that anticipate sudden deterioration rather than merely react to it.
More Figures (2)